The diagnosis is on the mycobacteria.
The infection that's been spreading throughout my right arm for at least three years has finally been identified. The lab report reads: *Mycobacterium chelonae/abcessus group.*
Surfing it up, I saw there are Issues about what its proper Latin name is. Exactly like with plants. (You've no idea what I waded through before I mentally tossed a coin and called my coontie *Zamila pumila aka Z. floridana.*)
The point is, as a rose by any other name...so is this bug. They know exactly what it is. Finally. Finally. This means we can tailor the treatment to kill it. It's not bad news to hear this. We already knew it was a nasty germ. It's really, really good to know precisely which nasty germ it is.
Right on the tail of that piece of news came another one.
My immune system is crashing.
A lot or a little, I don't yet know.
I've been immunocompromised for years because of taking high dose steroids. Prednisone. And just yesterday I found out that opioids are also immunosuppressants. I had no idea. I'm on 50mg Fentanyl patches and go through 40 5mg oxycodone per month, which could be enough for immunosuppression.
Here's the Prednisone history.
I became completely disabled from allergies in 1991. I didn't take any significant or steady amounts of Prednisone for many years, just short term for bad exacerbations, ER visits, like that. My then-RA doc and various allergists urged me to consider taking the high-dose treatment, and I refused for years, because of the side effects.
As time went on, I ended up spending more and more of my life sick in bed. Just from allergies, yes. They really are that bad. Toward the end of my pre-Prednisone days, I thought I was spending 6-8 months per year mostly bedridden. One day, accompanying me on a doctor visit, Walter gently corrected me and told the doc --No, it's actually about 10 months a year, she just doesn't realize it.
And I thought about that, and I knew he was right.
The toll on the body from being universally allergic is stunning. On my good days, it's like a constant case of really bad flu. Have you ever had that, where a bad flu goes on forever and you just can't function? Weak and congested everywhere and coughing and sneezing and itching and aching and can't stay awake. Just moving around is like dragging your limbs through water.
There were times I had to crawl to get to the bathroom. Adding insult to injury, that would hurt my dignity - and my arthritis and fibromyalgia and plantar fasciitis too. It hurts to crawl on tile floors. I laugh and snort at it all I can, but truly, it's not fun. Having to crawl just really gets my goat, it's a thing that's hard to take, hard to stay tough about.
Here's what was worse than any of that.
For a few years, I was blessed by the presence of my grandmother here, my father's mother Helen. I loved Helen. She was a fine artist, and had a pilot's license, and all sorts of other cool stuff. She lived in an assisted living facility in Boca Raton, not so far from me. I had no real responsibilities for her life's needs, just to visit her and have fun. She'd had a stroke which left her speech pretty badly impaired, but she was fairly ambulatory. And she was a joy to be around. She had a wicked sense of humor and a smile that lit up a room.
My father's family is from the Southwest, so when we moved to Illinois when I was 7, I didn't see much of them after that. I got my grandmother Helen here from her assisted living place in Phoenix only because her daughter Ruth died young (in her 60's) from a rare duodenal cancer. Ruth had been helping care for Helen.
But...I was so sick from allergies that sometimes two or three months would go by when I couldn't visit Helen. You see, I not only couldn't drive. I couldn't stay awake. Couldn't walk. I couldn't talk coherently. For me, breathing pollen-laden air is like breathing chloroform.
If I'd taken the Prednisone back then, I would have had so much more time with Helen. Wonderful time, fun time. I lost that and I'll never get it back. She died.
That's why I say my only regret about the steroids is not taking them sooner.
This is not to say I like the long-term damage it does. I'm perfectly aware of the side effects, and always have been. My grandfather Eddie, Helen's husband, was one of the earliest patients treated with steroids. Back in 1958 - the year I was born - he came down with a form of rheumatoid arthritis that was literally killing him. Since he was dying anyway, they gave him cortisone as an experimental treatment. It saved his life. I saw home movies of him throwing away his cane and silently laughing.
It also half-blinded him. They didn't know back then that you have to taper it off slowly. They just stopped it. He still drove a car, but his peripheral vision wasn't very good. My father the MD, and my mother's mother Jean, an RN, used to argue about whether it was the RA that got his eyes, or the steroid withdrawal.
With all the worsening infection issues in the past year or two, I've been slowly but surely decreasing my own Prednisone dose. To combat side effects, I take higher doses on alternate days, so one day will be a high dose day, the next lower, the next higher, like that. At its highest it was around 70 and 40 mg on alternate days. Now, I've got it down to 25, 35, 25,...And I think that's about as far down as I can go. At that dose, I can't move my hands much in the mornings for a good hour and a half. My fingers and wrists are totally stiff. The Pred doesn't just help with the allergies and asthma, but with the rheumatoid arthritis too. It helps it significantly.
Steroids have a lot of benefits for allergic people, of course. That's why they give it to you in the hospital to save your life if you're in anaphylaxis. Why they put it in EpiPens, *bee-sting kits,* like the ones I have scattered all over the house and my purse. And have had to use, twice.
At any rate: Now, for the first time, I'm measurably immunocompromised.
Immunoglobulins - *Ig* - are antibodies. There are five types: IgM, IgD, IgG, IgA, and IgE.
IgG provides antibodies to infection. IgE provides antibodies to allergens. So ideally, to treat allergies, you'd want to target IgE for suppression.
Prednisone, however, suppresses IgG more than IgE. There's no way I've heard of to suppress just IgE.
For the first time, my blood work has come back with a noticeable drop in IgG. It's 544, and the reference range Quest cited is 694 - 1618 mg/dL. So, I'm low.
How significantly low that is, I don't know yet. Or, how much we can do to combat it. I'll have a lot to discuss with the RA doc Monday and the ID doc Wednesday. And while they're both well versed in immunology, still, neither one is the best doc to address something this complicated. For example, maybe IgG booster shots would help. The ID doc doesn't do them. This is the purview of an allergist/immunologist.
When I googled IgG to read up on the effects of low IgG, suddenly so many things made sense. Here's some of the unusual symptoms I've been feeling over the past 6 months or so - symptoms common to low IgG patients:
-Chronic upper and lower respiratory infections of abnormal cause. Hello, weird lung infection and hospital stay. And terrible sore throat yesterday, red and inflamed, maybe thrush. We seem to have ruled out aspergillus for the lungs, and in the low IgG, found a reasonable explanation for what occurred. It matters less what germ it was. What got me so sick was that I couldn't fight most any germ - low IgG.
-Profound headaches. Strange new ones, quite different than I usually get - not a sinus, fever, TMJ, or tension headache. And these new ones are really severe.
-Constant ear infections. That's why I went to the ENT in my recent Doctor Daze week. Off and on, I've had terrible ear pressure problems for several months now, and my hearing's gotten really bad. The pain gets so intense I can't even blow bubbles into my ear like usual to clear the Eustachian tubes.
--Chronic skin infections. Recently, almost every time I went out in the yard, I'd wake up next day with another weird new skin problem. I'm fighting it with various precautions, and I am doing better, but to have this happen is a bit...sobering. Watching your skin burst out in weird red things for no real reason is like something in a horror movie.
--An increase in the *fever sickness,* that array of sweats and chills, fevers and dizziness; and in the blistering from the disseminated HSV it comes with. Lots of new oral blood blisters, lots of new toe blisters.
I just have no immunity to fight ordinary germs right now. The ones that live all around us and on us and in us, but never infect us, are infecting me.
My old allergist, a scientist down at Jackson in Miami, told me a few years ago there was nothing more she could do for me, and basically cut me loose. Just continue the treatment I was on, which my primary can oversee. For that place and time, she was right.
My new insurance only lets me see doctors in Broward County, so I couldn't get to her even if I wanted to. But I'd rather see someone new anyway. It's time for fresh blood. So I'm looking.
Back to the mycobacteria now.
I've had this thing for at least three years. It way predates my blog, which was 2 years old in early April. I remember crying on my blogdad's virtual shoulder about these bumps in my arm for perhaps as long as a year before the blog. And they were there for a while before I started to worry about them.
The mycobacterial infection is highly likely to have triggered the tenosynovitis that's partially crippled my right hand. It's not damaged all that much; it's just that the pinkie doesn't work right because the tendon is *dropped.* The hand has some numbness from the surgery to correct the first tenosynovitis; then, one week after that was pretty much healed, the next tendon over got it.
And that tendon, a second tendon for your pinkie finger, is so tiny and delicate - the size of a hair, I was told - that it's basically inoperable. So now I have the big scar and nerve damage from the first surgery, and the disfiguring big lump of tenosynovitis next tendon over, and a pinkie that doesn't work right.
Something I've only mentioned here in passing is that I speak ASL. Sign language for the deaf. I don't hang out with any *deafies* any more, being a hermit and all, but this was a significant part of my life for quite a while. I was a good signer. To me, ASL is the most beautiful language of all mankind.
And I can't speak it right any more and never will again. I sort of stutter, now, in sign language. That dropped tendon in the pinkie finger of my dominant hand does more than make me do typos on the keyboard here. It's had a significant and permanent effect on my life.
The myco also probably triggered the bursitis in my left elbow. Again, it's a big disfiguring lump. It's also quite painful. It's a kind of pain that gets in the way: every single time I get out of bed, that's the elbow I roll onto to get up. I garden sitting down, and that elbow comes into play in the yard. I have problems extending and bending it, and carrying things, despite the pain treatment. Pain treatment is never enough, folks, not nearly. It's just enough to take the edge off. On a *medium* or average type day, my pain level is around 6 or so - after treatment. (That would be a 9 to a lot of other people.)
Having your dominant arm compromised in both hand and elbow impacts your life. I'm not whining about it here, not yet at least. I'm just stating the facts, okay?
Now add in these lumps of the myco infection in my right arm lymphatics. If you've ever had swollen glands from a strep throat, or any of the other myriad ways your lymph nodes get swollen and tender, then you KNOW what I'm talking about. That shit HURTS.
A series of lumps, infected lymph nodes and also small cysts, runs from above the elbow all the way to my fingertips. Maybe five nodes are so large, and a bit red and scarred, that they're actually visible to the naked eye. By passing my hand over them I can count, today, about...twenty nodes and ten cysts. And I see another new cyst in my right hand.
In late 2005, I finally arm-twisted my vicious Medicare HMO into getting me to a REAL dermatologist - rather than their effing cosmeticians who wanted to *Rejuvenate my Hideous Sun-Damaged Skin!!!* That dermatologist was a true scientist. Another Jackson guy, triple board certified in dermatology, dermatopathology, and one other I can't remember now. Dr. K the World-Class Dermatologist. Literally. He works internationally. His CV is just stunning.
And he cultured one of the lumps. And got nothing.
Well, no culture. They did say it was a granulomatous infection and looked like mycobacteria, which could include TB, leprosy, or a whole slew of rare mycos.
Mycobacteria is extremely difficult to grow in culture, so a culture failure is the norm. Here's how kdad explained it. Remember, he's an MD scientist and microbiologist himself, and one who does a lot of tissue culture.
Myco is *slow growing* and *rare.* Even if you get a good sample, it takes forever for enough cells to grow so that you can actually see them. They are few and far between. So if you're willing to wait for 2 months trying to make it grow - as opposed to many cultures that grow in a few days - you MAY grow enough baby bacteria to see them in the medium in the petri dish, and put a little scraping on a slide and stick it in your microscope. But because they're rare - not many grow in those 2 months - you may move the slide around, looking and looking, and still not see them. They're there, though. So is a needle in a haystack.
He told me there's around a 10% success rate with myco cultures. This means that you will, eventually, get an answer. It means that culturing it over and over is NOT a waste of time; you keep going, and maybe the 10th time is a charm.
But it has to be a good lab, willing to stick with it. See, most labs will throw the culture away after two or four weeks, if it doesn't grow. Myco needs more time. The Quest special projects lab, kdad said, is a good one. Very good. They'll get the materials passed on to them after the local lab sees what they're looking at, and does the preliminary work.
The special lab may be great. However: both the local lab, and the local collection office, leave a great deal to be desired. IMO.
Dr. K in Miami got nothing on that first culture. About a year later, he tried again. Nothing.
I changed insurance and can't see him any more. The good news is, there's a great Broward dermatologist, Dr. G, I've wanted to see for years now. For the first time, he IS on my insurance, yay! AND, my wonderful ID doc does a lot of work with him, sending patients back and forth as they need. AND! As it turns out, the Miami World-Class Dermatologist Dr. K? He is Dr. G's old teacher, and his mentor.
Frankly...I like Dr. G better. He was wonderful when I went in. Fascinated with my case. That's the one where every time I go, his docs in training - he runs a residency program - all grab their digital cameras and take pix of my booboos. They especially like all the *staining,* what looks like bruises, on my legs.
Dr. G biopsied the right arm. He was looking for more than just myco, too; he wanted some interesting fungal tests done. Stuff that, to his glee, he found out Dr. K did NOT do. Man, I like that Dr. G!
He did 5 punches. This, remember, was my 3rd time trying to culture this bacteria.
When he sent the tissue samples to Quest, he did the paperwork with great care, partly because he was putting some duplicate samples in the same vials.
And when Quest got them - they threw 4 of the samples away.
Yes. You read right.
They THREW THEM AWAY.
We were all furious, but what can you do? They're gone.
Quest did 2 of the 5 tests on the one specimen they deigned to keep. That meant we only had to repeat 3 of the punches.
So I went back for the 4th set of biopsies.
This is extremely tender tissue here, folks. I mean, it hurts just amazingly. I rest my arm on my workstation on these infected lumps and it's an issue every single time I write a post or comment. Bet you didn't know that, huh?
Since I have fibromyalgia, and thus a seriously overdeveloped pain nerve network, the docs kindly use extra Novocaine. They'll use 10 or 20 shots. That helps. After the first few I don't always feel the needle going in.
What they use to take samples is either a scalpel or a hollow tube, like a little straw, a bit bigger in cross section than an old-fashioned coffee stirrer stick. That red and white striped plastic straw we used to see in the break room at work, don't know if they're still out there or not, I'm a hermit now and have no familiarity with such things any more.
The end is scalpel-sharp. They *punch* it into your skin, dig around to get up to a good half-inch or so of tissue, then take it out of the tube and into a vial for the lab.
My first biopsy in Miami? They just used a scalpel and cut out a big chunk, and stitched it back up, in two different places. One site looked like my disseminated HSV-1 (systemic cold sores); we wanted some proof. It was. One down.
The second Miami biopsy? Just the one sample cut into more than one piece, so a fairly big scalpel chunk, stitched up.
The first Broward culture was five punches, from two different sites. By now they're seeing way too much infection with me, so for safety, to keep it open and draining, they didn't stitch it. That way it leaves big ol' scars, but at least you're less likely to lose your arm to an infection.
To take biopsies from a CA MRSA carrier is a very dangerous thing to do, even once. Cut my skin, and it gets infected. One day, the infection will win, and it'll all be over.
The second Broward culture was three punches, all from the same site.
Most of those eight punches came out of the same giant-sized infected lymph node. It's gone down now, finally, swelling wise. I had three really big nodes around there and they're all smaller. It looks like the permanent antibiotic cocktail I'm on is helping.
Unfortunately...at the same time, I have new infected nodes toward my wrist. One especially, all big and tender. Not good. This bacterial infection shouldn't be spreading in the presence of all that Cipro and minocycline I'm taking every day now.
Okay. The biopsies are done and the cultures are trying to grow. Now, we wait...
2 weeks? nothing...
4 weeks? nothing...
6 weeks? nothing...
8 weeks? nothing...
and the lab is giving up and throwing them away. Again.
I saw Dr. G a couple weeks ago, on that big Doctor Daze week I had. He suggested getting with Dr. C (ID doc) and trying some antifungal treatment, since it had the appearance, at least, of sporotrichosis, a fungal infection. He said, --Since we can't get a culture, let's not let time go by when we can try to treat it based on an empirical diagnosis. I'll coordinate with Dr. C.
Okay.
My appointment with Dr. C was the next week.
Between those two appointments, another lab result came through.
Quest identified it.
Not by culturing it in a petri dish.
They - get this - they DNA sequenced it.
They put a polite note at the bottom of the lab report explaining how this was not an FDA approved method.
I couldn't possibly care less.
We know what it is.
And we know for sure, now, that it's not leprosy or TB. And I'm so very grateful for that.
I was in the office, waiting for her in an exam room, when Dr. C got the fax for the first time. She came in with a barely subdued sense of excitement, intensely focused. She tried calling Quest to get some more info, but the special lab's in CA and they weren't in yet.
And the minute she saw the name she said, --Ah! Yes. That's very much in keeping with its looks and behavior. This result makes sense to me.-- She's right, too. I googled it.
And one of the characteristic things it does? It looks like...sporotrichosis.
But it's not.
It makes subcutaneous abscesses and infects your lymph nodes. It's, relatively, a fast growing mycobacteria. I described it in an earlier post as a *slow crawl,* talking about how different it looked from the way MRSA spreads.
Dr. C knew, all along, that it wasn't my usual CA MRSA. Dr. K in Miami called it wrong; he thought it was MRSA.
Dr. C wondered if it might be sporotrichosis, but was resevered in her opinion. Dr. G, the Broward dermatologist, was convinced enough that he was ready to start antifungals.
He called it wrong, too.
Dr. C the ID doc? OH, she RULES.
She proposes the following treatment. First, we want to add a 3rd antibiotic to my cocktail. Since I'm so allergic, including to antibiotics, she wants to be safe. She asked me about my reactions to the various allergenic antibiotics on my list, and I told her. There are a couple that are good on this particular myco that I've never tried, so maybe I'm not allergic to those. I also told her that as much as I sensitize to new things, I also DEsensitize over time. So I'm actually willing to try anything except penicillin, even if I reacted to it before.
She said, Okay. She's going to research and think and come up with the most ideal 3rd antibiotic she can. And: put me in the hospital for 24 hours for the first two doses, just for observation, just in case I do react to it.
This, for an ORAL antibiotic.
I really like her style. She's keeping me safe.
Now: Ideally, you want to do a sensitivity test on the germ. Once you culture it, you put it together with different types of antibiotics and see exactly what kills it the best. That's the antibiotic you give the patient.
However: since they DNA sequenced it, instead of growing it in culture, I think that's not gonna happen. And I think that's what she was calling Quest about.
What she wanted to do was see if it was sensitive to at least 2 of the 3 antibiotics she'll have me on. If so? Keep those three. If it were sensitive to only 1, or none? Change them.
Smart plan. Great plan. But...no culture, no can do.
So we'll have to wing it.
And, perhaps, try some IgG booster too.
I've been waiting for this day for a long, long time. For both questions: learning the bad news about the immune system crash, and also, learning what that myco infection really was.
Somehow, though, I'm not as prepared as I thought I would be.
~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~
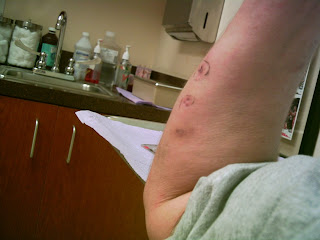
Mark your Target and Shoot: They like to draw outlines on me with a pen. Here, it's to remind the doctor where she found good sources for the biopsies. She'll narrow it down as she goes.

Novocaine.

More novocaine.

Lots and lots of novocaine. This went on for quite a while.
Sometimes after a session like this, I have wasp dreams that night.

8 comments:
Congrats on the identification!
I'm so sorry about the immunity issue.
Sometimes I feel like a hypochondriac when I read about you and that scares the shit outta me.
But I'm so grateful to you for putting it all out there to help others.
I just wish there was more I could do for you my friend. Hugs
And the thought just occurred to me... with your severe allergies, why are you not on an oxygen mask 24/7?
Don't take a genius to figure out that's healthier for you than breathing contaminated air.
I'll be all right! I always am in the end. And you are NO hypochondriac, you. I feel lucky compared to you. No cancer, hardly missing parts, just gall bladder really.
This cracks me up. We each think the other is worse off!
I would adore to be on oxygen 24/7, for exactly the reason you said. Also, apparently, there's even a different physical mechanism that decreases allergic response when you feed in oxygen. My RA doc told me about it, I didn't take notes so I don't remember how it works. I want to ask him again tomorrow.
The only and only reason I can't get oxygen is because the insurance refuses to pay for it unless I have COPD. And since I basically *cured* it - meaning, just got it under good control cause it's NOT curable!!! - now, I can't get oxygen.
And I can't afford to pay for it myself.
So...I think that may be one of my upcoming health projects this year. I really need it, big time, and maybe - maybe - I can get some under a Patient Assistance program of some kind. Two of my docs already agreed to write the scripts, so that's good, that's half the battle right there.
K, you are an inspiration to anyone who ever thought of giving up.
God Bless You. I'll be keeping you in my prayers.
(((hugs))) ditto to what kdzu said... you are definitely one of my heroes! (((hugs))) hang in there.... I can, however, unfortunately relate to the plantar faciitis thing you mentioned - I've got a pretty bad case of it, and walking and standing for ANY length of time is AGONY. It's improved some, but not enough yet... I can't imagine having to cope with it, on top of other conditions, too.
haha I will prove you are worse when we meet! LOL I forgot I have plantar fasciitis too! Very high arches. I've found that wearing those ankles braces from Walmart to bed helps a lot.
The way my PT explained it... when we sleep our feet are always in a pointed position which shortens our achilles tendon. By wearing the braces to bed, they keep the feet in a flexed position, thereby stretching the achilles tendon.
Echoing here what kdzu says. If there is anything I can do to help, please let me know. ((hugs))
I love you guys.
You know, I used to sleep with my *night splint* all the time. I only got one, from the doc, since they feet got the fasciitis one at a time. He explained it exactly like yours did, why it works.
Then they got better so I stopped. Now they're bad again that way.
duhhhhh!!!!!
guess who's gonna dig out that night splint again tonight?!
Livey, those very high arches? In my family we have to be really careful who we date. ;-)
Post a Comment